One of the most common fears patients express is this:
“Is this going to spread?”
“Will this reach my brain?”
“Can neuropathy damage my heart?”
These are understandable concerns.
The word “nerve damage” sounds systemic and progressive.
Let’s clarify this carefully.
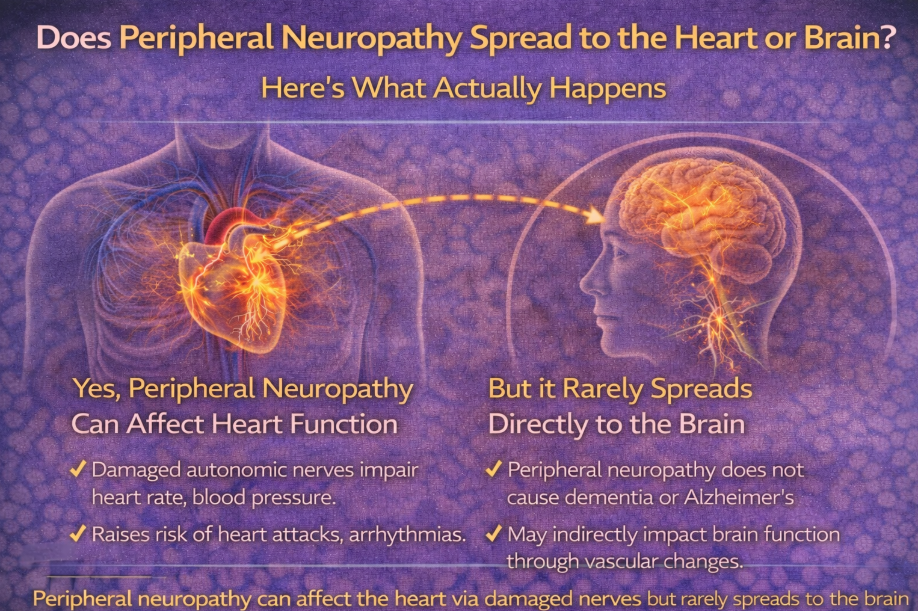
Peripheral neuropathy does not spread to the brain.
It does not directly damage the heart muscle.
But there are important distinctions worth understanding.
What Peripheral Neuropathy Actually Affects
Peripheral neuropathy involves nerves outside the brain and spinal cord.
These peripheral nerves control:
- Sensation
- Muscle movement
- Autonomic regulation (blood pressure, digestion, heart rate variability)
By definition, peripheral neuropathy does not involve the brain.
If the brain or spinal cord were affected, the condition would be classified differently (central nervous system disorder).
Peripheral means outside the central nervous system.¹
Can Neuropathy Travel to the Brain?
No.
Peripheral neuropathy does not “spread upward” into the brain.
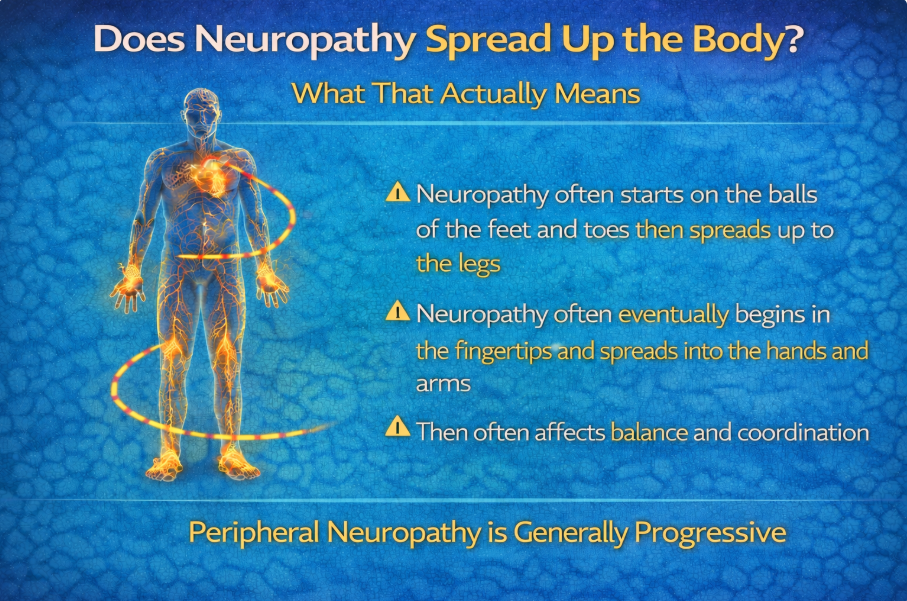
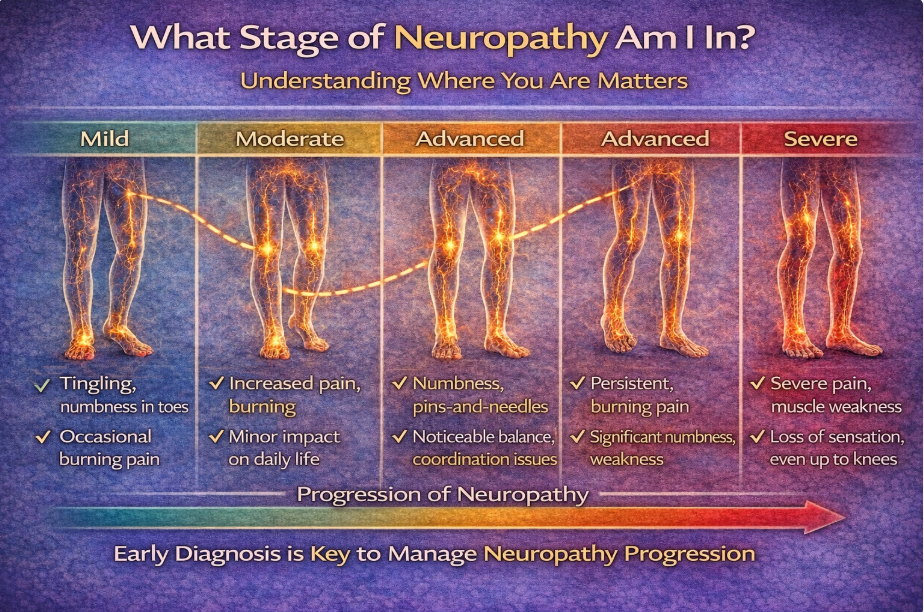
Symptoms may progress from the toes toward the legs in a length-dependent pattern.
But that reflects vulnerability of longer nerve fibers — not migration toward the brain.²
Neuropathy progression follows anatomical patterns, not a spreading infection.
What About the Heart?
This is where nuance matters.
Peripheral neuropathy does not damage the heart muscle itself.
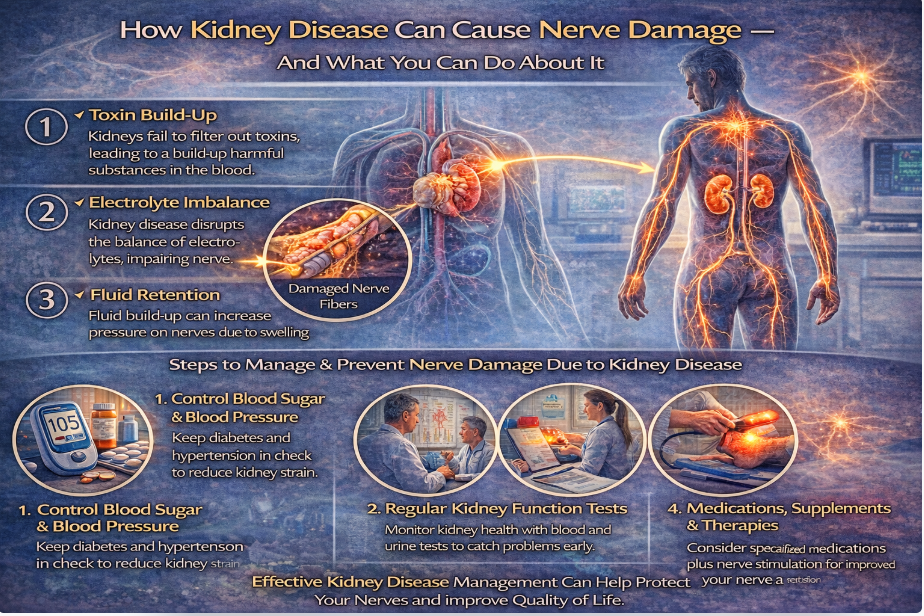
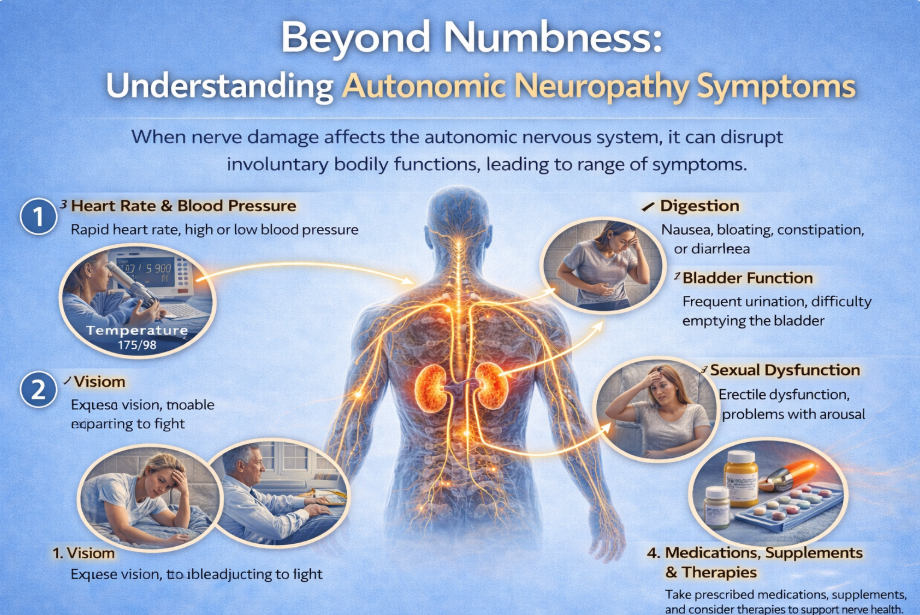
However, certain forms of neuropathy can affect autonomic nerves.
Autonomic nerves help regulate:
- Heart rate
- Blood pressure
- Heart rate variability
This is called autonomic neuropathy.
In long-standing diabetes or systemic disease, autonomic involvement can influence cardiovascular regulation.³
That does not mean neuropathy attacks the heart muscle.
It means the regulatory signals may be altered.
When Is Autonomic Neuropathy Concerning?
Autonomic involvement becomes more concerning when symptoms include:
- Recurrent fainting
- Severe orthostatic hypotension (blood pressure drops when standing)
- Persistent abnormal heart rate patterns
These are typically associated with long-standing systemic disease — not mild peripheral neuropathy.
Autonomic neuropathy is part of broader metabolic or systemic stress, not an isolated spreading nerve condition.
Does Neuropathy Reach the Brain in Severe Cases?
Peripheral neuropathy does not become a brain disease.
However, symptoms like:
- Dizziness
- Lightheadedness
- Balance instability
may feel neurological in a broader sense.
Balance changes in neuropathy are due to reduced sensory input from the feet — not damage to the brain.⁴
The brain simply receives incomplete information.
That distinction is important.
Why Symptoms Can Feel Like They’re Spreading
Patients often describe symptoms as:
- “Climbing up my legs”
- “Moving higher”
- “Getting closer to my body”
This reflects length-dependent nerve involvement.
Longer nerves are more metabolically vulnerable.
So symptoms move from toes → feet → calves.
This is predictable anatomy, not systemic invasion.
When You Should Seek Immediate Evaluation
While peripheral neuropathy does not spread to the brain, certain symptoms require urgent medical evaluation:
- Sudden weakness
- Loss of bowel or bladder control
- Severe new neurological changes
- Rapidly progressive paralysis
These are not typical peripheral neuropathy symptoms.
They may reflect different neurological conditions.
Chronic neuropathy develops gradually.
Rapid neurological changes are a separate category.
The Most Important Takeaway
Peripheral neuropathy does not spread to the brain.
It does not directly damage the heart muscle.
Autonomic neuropathy can influence heart rate and blood pressure regulation in systemic conditions — but it is not a migrating nerve disease.
Understanding anatomy reduces unnecessary fear.
Clarity prevents catastrophic thinking.
Frequently Asked Questions
Q: Can neuropathy travel to the brain?
A: No. Peripheral neuropathy affects nerves outside the brain and spinal cord.
Q: Can neuropathy damage the heart?
A: Peripheral neuropathy does not damage the heart muscle. Autonomic neuropathy may influence heart rate regulation in systemic disease.
Q: What is autonomic neuropathy?
A: Autonomic neuropathy affects nerves that regulate involuntary functions such as heart rate and blood pressure.
Q: Should I worry about neuropathy spreading?
A: Neuropathy may progress gradually along length-dependent nerve pathways, but it does not spread to the brain.
How This Connects to Prognosis
If you are concerned about life expectancy or long-term outcomes, read our full guide:
“What Is the Life Expectancy of a Person With Neuropathy?”
(Internal link to Pillar Article)
Next Step
If you are experiencing symptoms such as lightheadedness, heart rate irregularity, increasing instability, or new neurological changes, a structured neuropathy evaluation can help clarify whether autonomic involvement or overlapping conditions are present.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Early clarity can influence long-term trajectory and peace of mind.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
- England JD et al. Distal symmetric polyneuropathy. Neurology.
- American Academy of Neurology. Peripheral neuropathy overview.
- Vinik AI et al. Diabetic autonomic neuropathy. Diabetes Care.
- Richardson JK. Peripheral neuropathy and balance dysfunction. Mayo Clinic Proceedings.