Many patients searching for neuropathy treatment eventually ask:
“Does laser therapy actually work?”
The honest answer is:
Laser therapy is not a miracle cure.
But in structured, stage-appropriate protocols, it may support measurable improvement in nerve function.
Understanding what it can — and cannot — do is important.
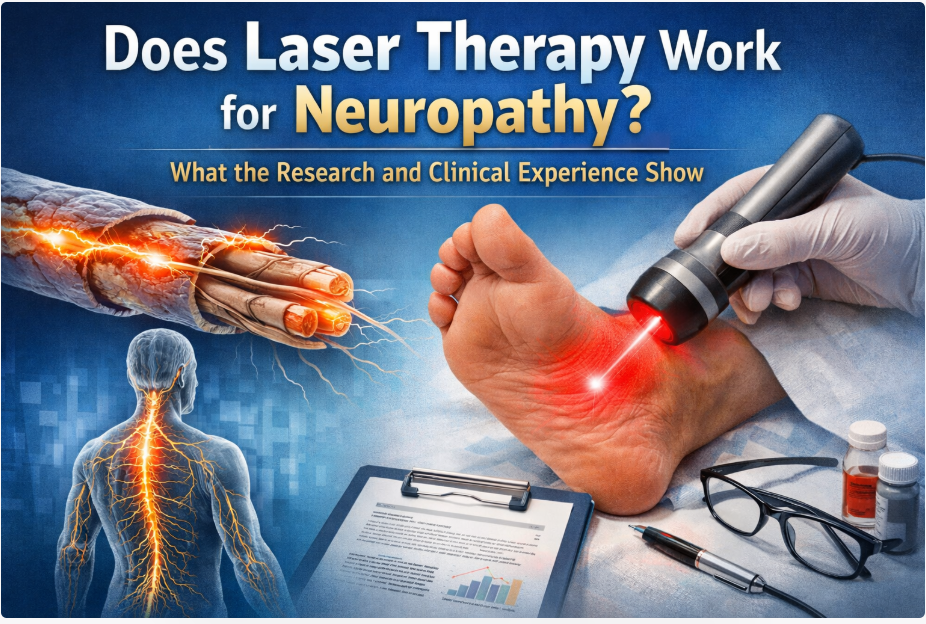
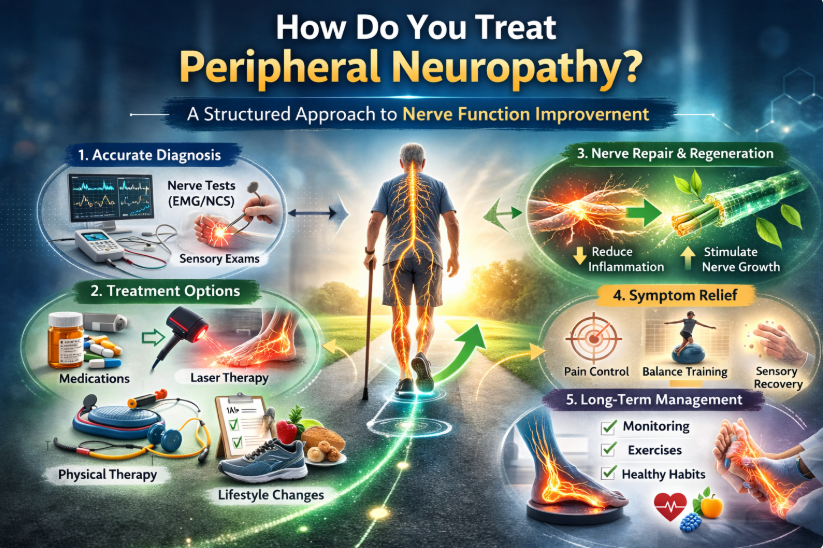
What Is Laser Therapy for Neuropathy?
Laser therapy used in neuropathy care is typically called:
Photobiomodulation (PBM)
Class IV medical lasers deliver specific wavelengths of light into tissue with the goal of influencing:
- Mitochondrial energy production
- Microcirculation
- Cellular signaling
- Inflammatory pathways
Unlike medications, which primarily suppress pain signals, laser therapy aims to influence the biological environment of the nerve itself.
What Does the Research Say?
Research in photobiomodulation suggests potential benefits such as:
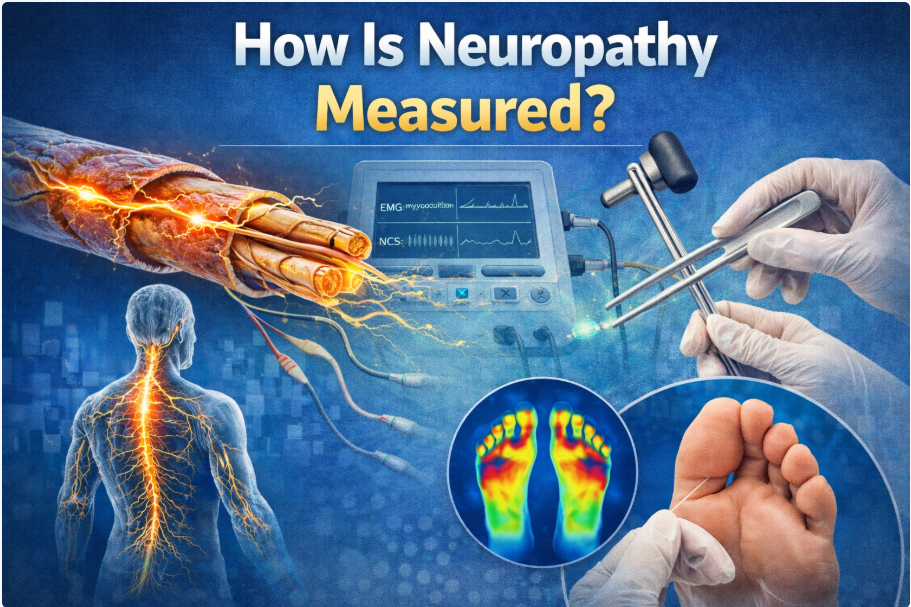
- Improved nerve conduction velocity
- Enhanced mitochondrial function
- Increased ATP production
- Reduced inflammatory signaling
Several studies have demonstrated improvement in sensory detection and nerve performance in certain neuropathy populations.¹
However:
Results vary by stage, severity, and consistency of treatment.
Laser therapy is not a guaranteed reversal.
It is a biological support intervention.
Pain Relief vs. Functional Improvement
An important distinction:
Many neuropathy treatments focus primarily on reducing pain.
But not all neuropathy is painful.
In over 20 years of focused neuropathy practice, a significant number of patients seeking care report:
- Minimal pain
- Intermittent discomfort
- Or no pain at all
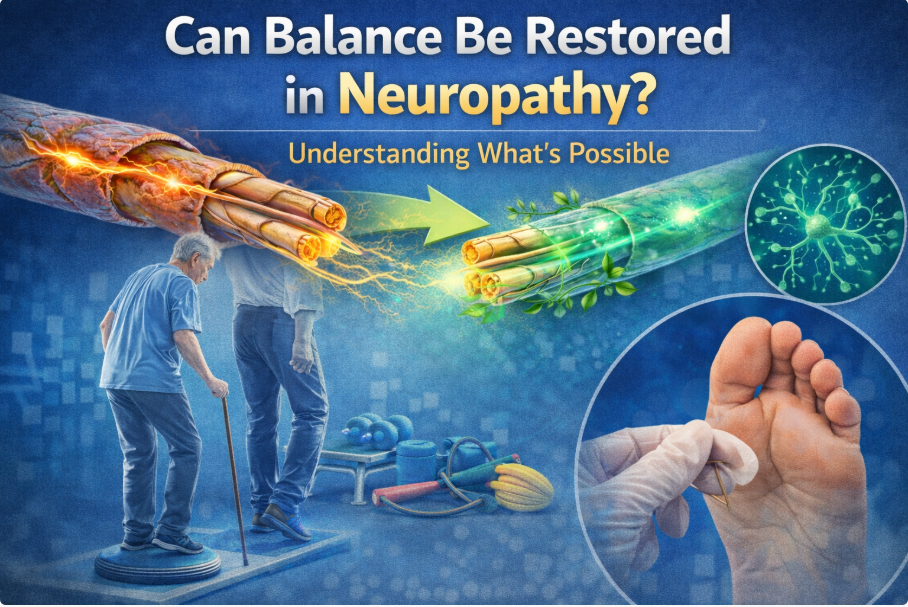
Instead, their primary concerns are:
- Balance instability
- Weakness
- Reduced walking endurance
- Tightness
- Fear of falling
Laser therapy is often marketed as a pain solution.
But in structured neuropathy care, the more important goal may be improving measurable nerve performance.
Pain reduction alone does not restore:
- Sensory detection
- Balance correction
- Strength output
Functional improvement requires a broader strategy.
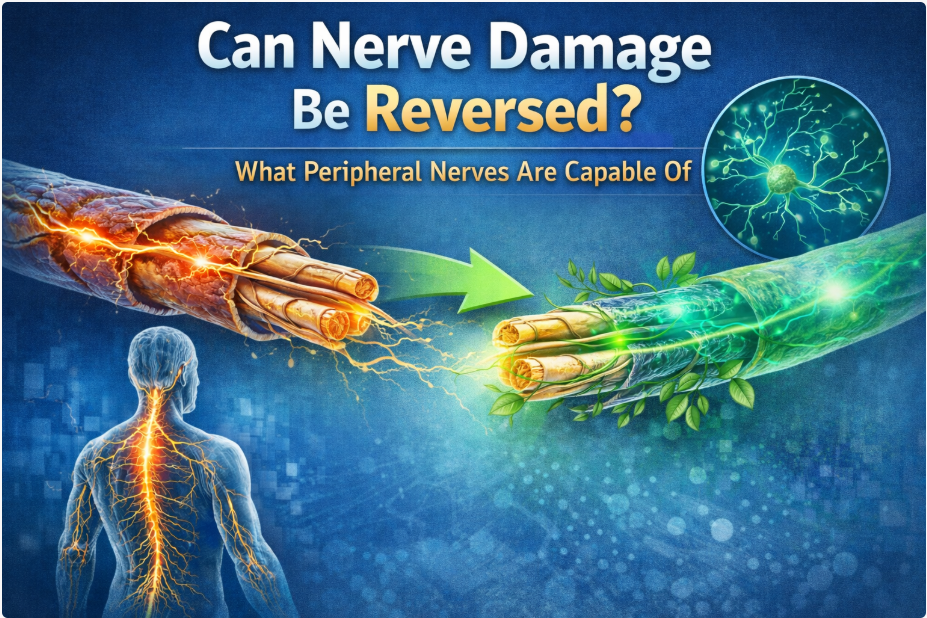
Can Laser Therapy Regenerate Nerves?
Peripheral nerves have regenerative capacity.
For a deeper explanation, see:
Can Nerve Damage Be Reversed?
Laser therapy may support:
- Cellular energy production
- Blood flow
- Nerve signaling efficiency
However, complete anatomical reversal is not guaranteed in chronic cases.
The realistic goal is measurable improvement — not instant cure.
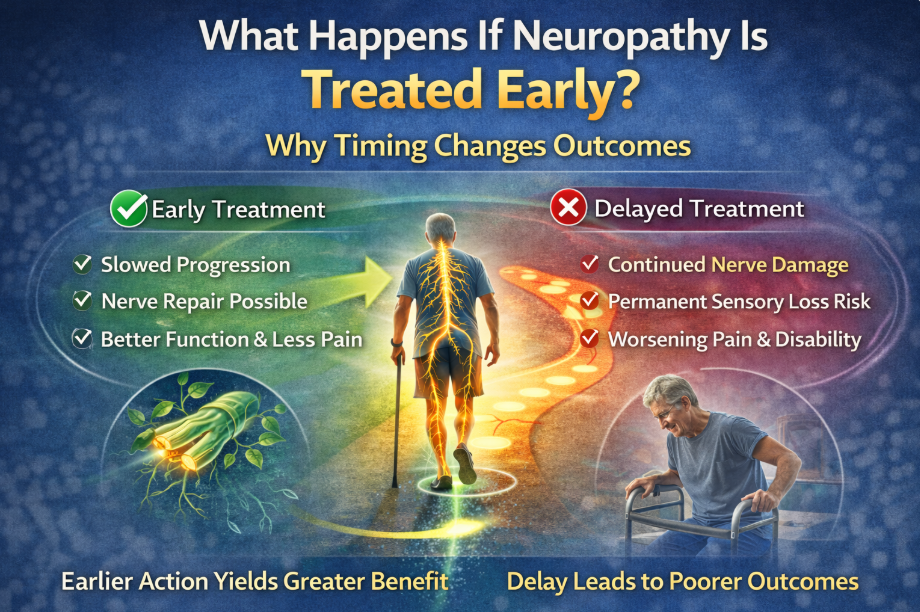
Does Stage Matter?
Yes.
Earlier-stage neuropathy tends to respond more predictably.
For staging clarity, see:
What Stage of Neuropathy Am I In?
When neuropathy is advanced and deconditioning is significant, laser therapy alone is rarely sufficient.
Patients may also need:
- Progressive walking
- Strength rebuilding
- Balance reinforcement
- Functional movement training
Strength and stability can improve — but consistency matters.
Laser therapy works best as part of a structured, comprehensive plan.
Is It Better Than Medication?
Medication and laser therapy serve different purposes.
Medications typically:
- Reduce pain perception
- Do not restore measurable nerve function
Laser therapy aims to:
- Influence nerve biology
- Support measurable sensory improvement
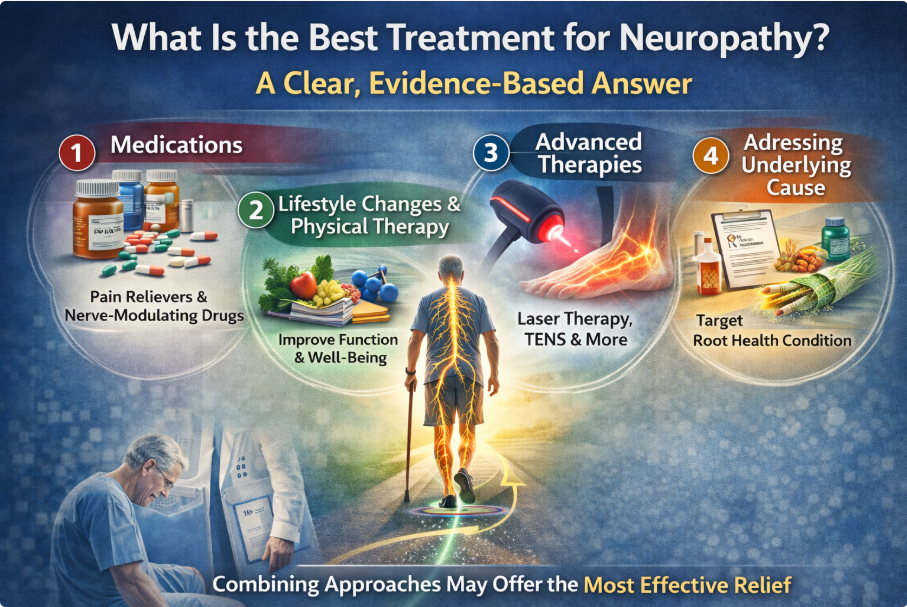
For a broader overview of treatment options, see:
What Is the Best Treatment for Neuropathy?
The best approach depends on the goal.
Comfort and function are not identical.
What Should Patients Realistically Expect?
Patients considering laser therapy should expect:
- Gradual change
- Measurable tracking
- Structured protocol
- Reinforcement with movement and balance work
Improvement is typically progressive — not immediate.
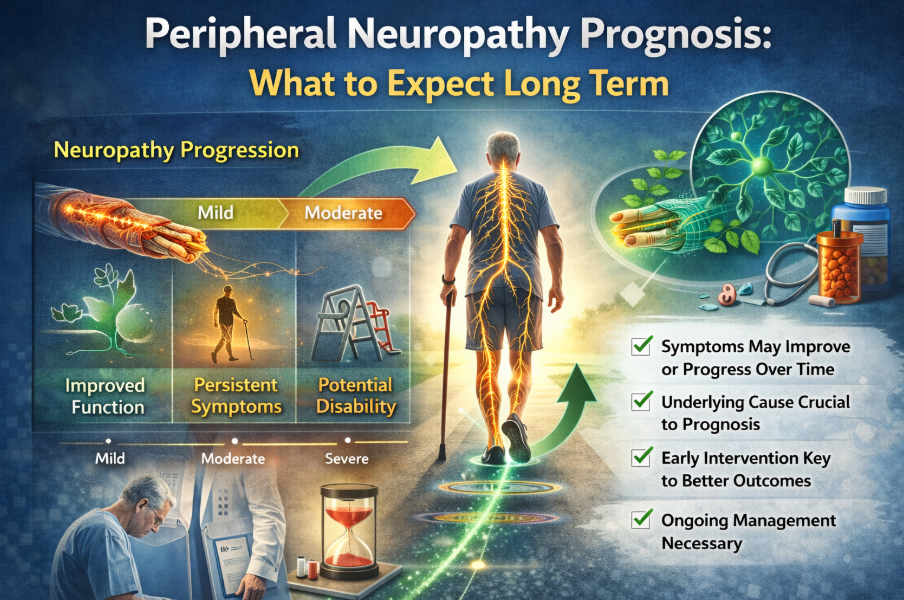
Untreated neuropathy commonly progresses.
For more on progression, see:
Is Neuropathy a Progressive Disease?
Laser therapy is not about hype.
It is about influencing trajectory.
The Most Important Takeaway
Laser therapy is not a miracle cure.
But when applied in structured, stage-appropriate protocols, it may support measurable improvement in nerve function.
Many neuropathy interventions focus only on pain.
Many patients are more concerned about balance and strength than pain.
Peripheral nerves retain capacity for improvement.
Earlier intervention tends to produce more predictable gains.
Laser therapy works best as part of a comprehensive plan aimed at restoring function — not just suppressing symptoms.
Frequently Asked Questions
Does laser therapy cure neuropathy?
No. It may support measurable improvement but is not a guaranteed cure.
How long does it take to see results?
Improvement timelines vary by stage and severity.
Is it safe?
When administered appropriately, medical-grade photobiomodulation is generally well tolerated.
Does it only help pain?
No. The goal may include improving measurable nerve function, not just pain reduction.
Next Step
If neuropathy symptoms are affecting sensation, balance, or endurance — whether painful or not — structured evaluation can determine whether laser therapy may be appropriate for your stage.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
The goal is not hype.
The goal is functional improvement.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
Hamblin MR. Photobiomodulation for peripheral nerve injury. Photomed Laser Surg.