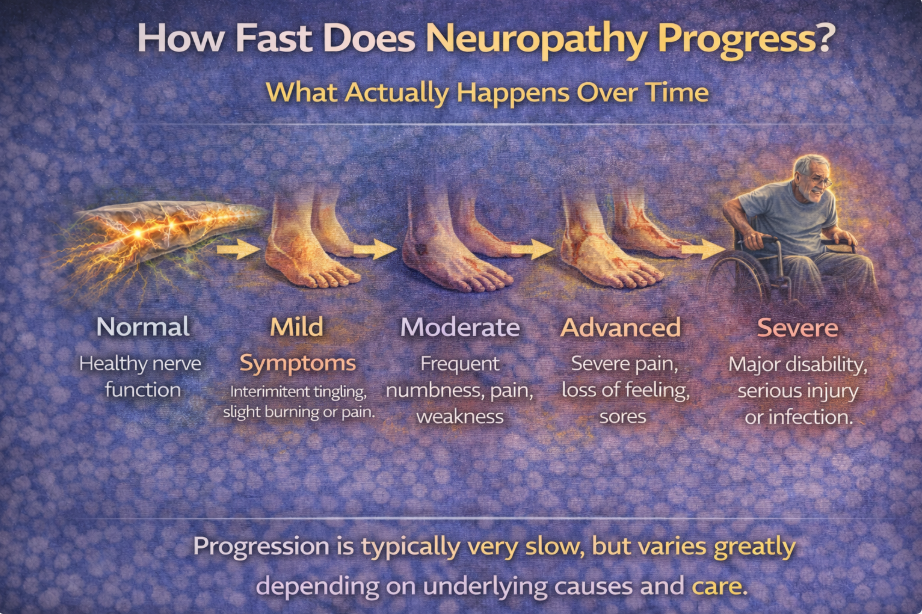
Peripheral neuropathy is not a single disease.
It is a condition that occurs when peripheral nerves are damaged or stressed.
That damage can happen for many different reasons.
Understanding the cause is important — but the cause does not always determine the outcome.
What Are Peripheral Nerves?
Peripheral nerves carry information between:
- The brain
- The spinal cord
- The muscles
- The skin
- The organs
They control:
- Sensation
- Movement
- Balance
- Temperature detection
- Reflexes
When these nerves are affected, symptoms may include:
- Numbness
- Tingling
- Burning
- Weakness
- Instability
The Most Common Causes of Neuropathy
Neuropathy can develop from several broad categories of stress.
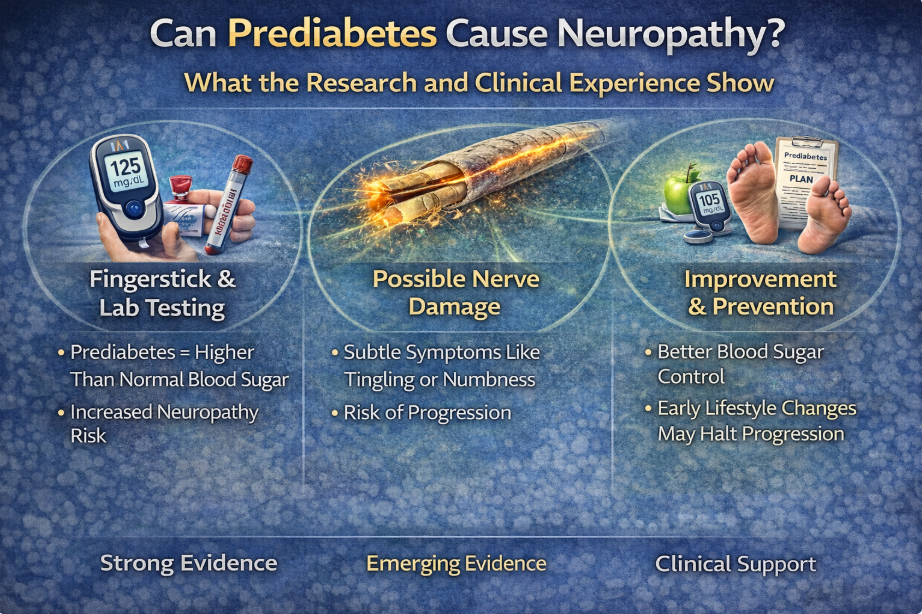
- Diabetes and Prediabetes
This is the most common cause of neuropathy in the United States.
Chronically elevated blood sugar can:
- Disrupt small blood vessels
- Impair nerve nutrition
- Increase oxidative stress
- Damage nerve fibers over time
Even mild blood sugar elevation (prediabetes) may contribute to nerve dysfunction.
For more on this, see: Can Prediabetes Cause Neuropathy?
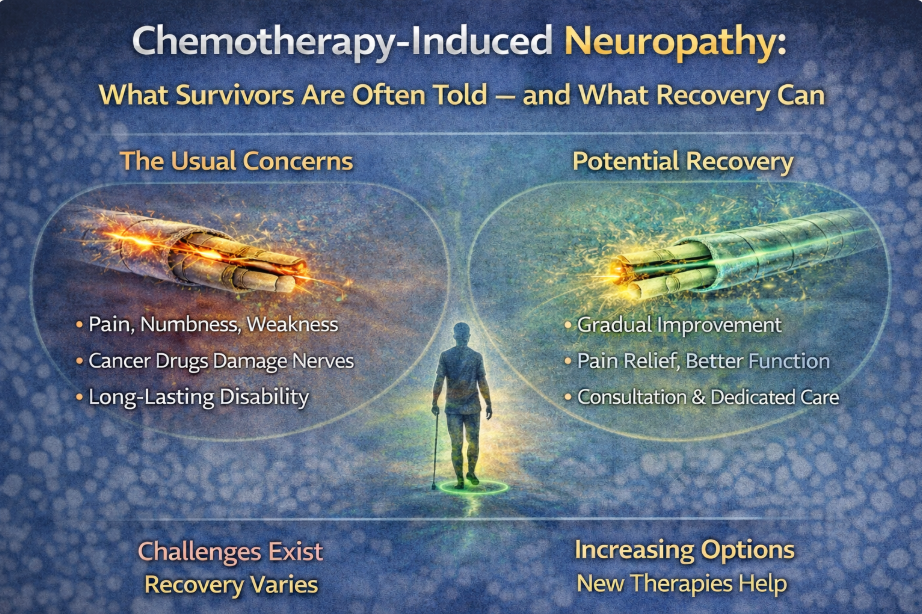
- Chemotherapy
Certain chemotherapy agents can directly affect peripheral nerves.
This is called:
Chemotherapy-Induced Peripheral Neuropathy (CIPN)
It may develop during or after treatment.
For more detail, see: Chemotherapy-Induced Neuropathy
- Vitamin Deficiencies
Low levels of certain vitamins — especially B12 — can impair nerve health.
When identified early, deficiency-related neuropathy may improve significantly with correction.
- Autoimmune Conditions
Some neuropathies occur when the immune system mistakenly attacks nerve tissue.
Examples include:
- CIDP
- Lupus-related neuropathy
- Sjögren’s syndrome
For more on autoimmune neuropathy, see: Autoimmune Neuropathy
- Alcohol-Related Nerve Damage
Long-term excessive alcohol use can:
- Impair nutrient absorption
- Increase nerve toxicity
- Contribute to progressive sensory loss
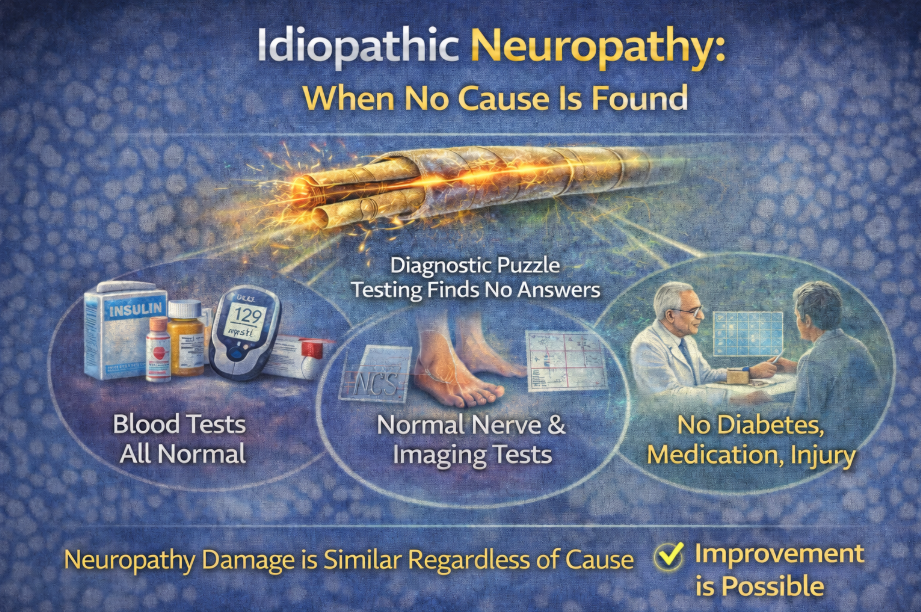
- Idiopathic Neuropathy
In many cases — sometimes up to 30–40% — no clear cause is identified.
This is called:
Idiopathic neuropathy.
For more on this, see: Idiopathic Neuropathy: When No Cause Is Found
Not having a known cause does not mean improvement is impossible.
Does the Cause Change the Treatment?
Identifying the cause is important for:
- Slowing progression
- Managing systemic health
- Preventing additional nerve stress
But in over 20 years of focused neuropathy practice, measurable nerve improvement is often possible regardless of the original trigger.
The cause explains why neuropathy started.
It does not always define how much recovery is possible.
For more on treatment strategies, see: What Is the Best Treatment for Neuropathy?
Can Neuropathy Have Multiple Causes?
Yes.
Many patients have overlapping contributors such as:
- Prediabetes
- Mild vitamin deficiency
- Age-related vascular change
- Medication exposure
Neuropathy is often multifactorial.
That is why structured evaluation is important.
Why Diagnosis Matters — But Isn’t the Whole Story
Medical diagnosis helps identify contributing factors.
But neuropathy care should also focus on:
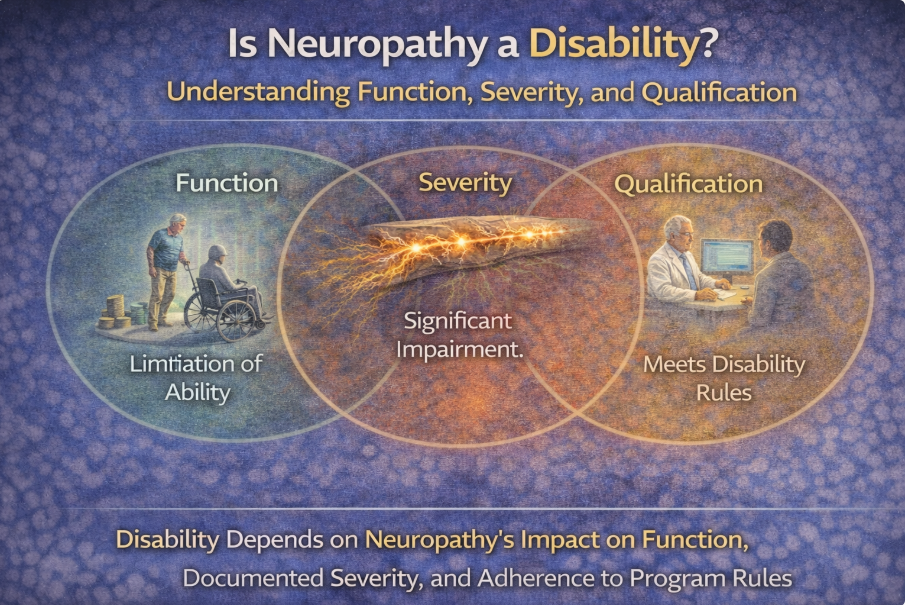
- Measuring severity
- Tracking progression
- Evaluating balance
- Assessing strength
- Monitoring sensory thresholds
For more on how neuropathy is measured, see: How Is Neuropathy Measured?
Diagnosis clarifies origin.
Measurement clarifies function.
Both matter.
The Most Important Takeaway
Peripheral neuropathy has many potential causes.
The most common include:
- Diabetes
- Prediabetes
- Chemotherapy
- Vitamin deficiency
- Autoimmune conditions
- Alcohol exposure
- Unknown (idiopathic) factors
Identifying the cause helps guide management.
But the presence of a cause does not automatically determine outcome.
Peripheral nerves retain capacity for measurable improvement.
Timing matters.
Structured care matters.
Frequently Asked Questions
What is the most common cause of neuropathy?
Diabetes is the most common cause in the United States.
Can neuropathy occur without diabetes?
Yes. Many cases are unrelated to diabetes.
Is idiopathic neuropathy untreatable?
No. Even when the cause is unknown, measurable improvement may still be possible.
Can multiple causes contribute at once?
Yes. Neuropathy is often multifactorial.
Next Step
If you have been diagnosed with neuropathy — or suspect early symptoms — structured evaluation can clarify both cause and functional stage.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Understanding the cause is important.
Measuring the function is essential.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.