Many patients say the same thing:
“It’s tolerable during the day… but at night it’s worse.”
Burning increases.
Tingling becomes more noticeable.
Tightness intensifies.
Sleep becomes disrupted.
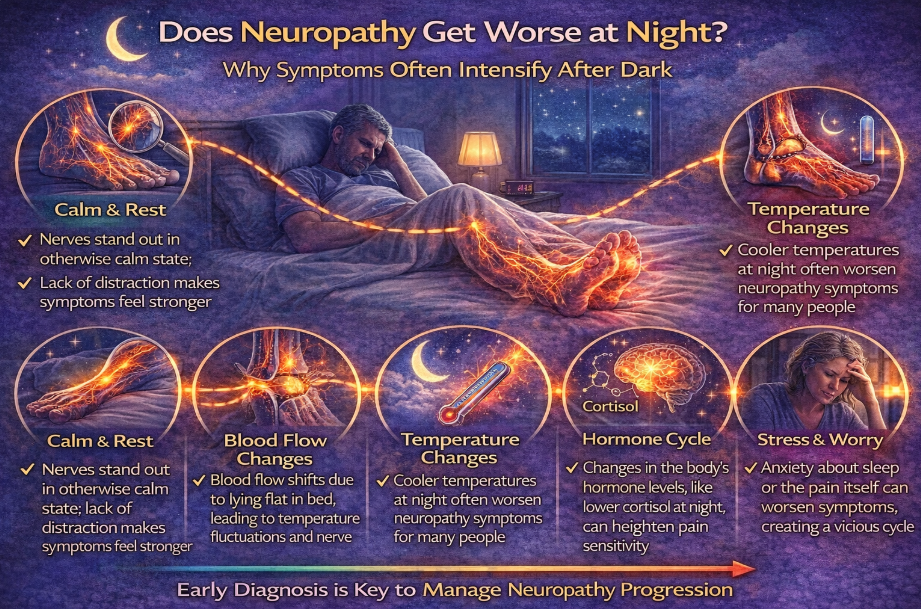
So why does neuropathy often feel worse at night?
The answer involves physiology, perception, and nerve sensitivity.
Why Symptoms Feel Stronger at Night
Neuropathy itself does not suddenly worsen after sunset.
But several factors make symptoms more noticeable in the evening.
1. Reduced Distraction
During the day:
- Movement stimulates circulation
- The brain is occupied
- Environmental input competes with pain signals
At night:
- The environment becomes quiet
- Attention shifts inward
- Sensory input decreases
When the brain has fewer competing signals, neuropathic sensations become more prominent.
2. Decreased Circulation During Rest
When lying still for extended periods:
- Circulation slows
- Nerve sensitivity may increase
- Tightness becomes more apparent
Movement supports nerve health.
Prolonged stillness can amplify symptom perception.
3. Circadian Pain Sensitivity
Research shows that pain perception follows circadian rhythms.²
Neuropathic pain may intensify at night due to:
- Hormonal shifts
- Reduced cortisol
- Increased inflammatory sensitivity
This does not mean nerves are suddenly worsening.
It means perception changes.
4. Autonomic Influence
In some patients, autonomic nerve involvement affects:
- Temperature regulation
- Vascular tone
- Peripheral blood flow
At night, altered regulation may contribute to:
- Burning sensations
- Heat sensitivity
- Tightness in calves and arches
For more on autonomic involvement, see:
Does Neuropathy Spread to the Heart or Brain?
Is Nighttime Worsening a Sign of Progression?
Not necessarily.
Nighttime symptom intensity does not automatically mean neuropathy is advancing.
However, if:
- Burning is increasing month-to-month
- Sleep disruption is worsening
- Balance is changing
- Sensation is decreasing
Those patterns may reflect progression rather than circadian fluctuation.
For more on progression timelines, see:
How Fast Does Neuropathy Progress?
Why Sleep Disruption Matters
Even though neuropathy rarely shortens lifespan directly, sleep disruption has meaningful impact on quality of life.
Chronic poor sleep contributes to:
- Increased pain sensitivity
- Fatigue
- Reduced daytime activity
- Slower reflexes
- Increased fall risk
When neuropathy disrupts sleep, functional decline can accelerate.
That is one way neuropathy affects daily life long before it affects survival.
For more on safety concerns, see:
When Is Neuropathy Dangerous?
Can Nighttime Symptoms Improve?
Yes.
Peripheral nerve function is not fixed.
In clinical practice, improvement may include:
- Reduced nighttime burning
- Improved sensory detection
- Decreased calf tightness
- Better sleep continuity
- Increased tolerance for rest without symptom flare
Earlier-stage neuropathy tends to respond more predictably than advanced-stage neuropathy.
For more on staging, see:
What Stage of Neuropathy Am I In?
Untreated neuropathy often progresses.
But measurable nerve function improvement is achievable when structured intervention begins earlier rather than later.
Practical Strategies for Nighttime Relief
While structured care addresses underlying nerve function, patients can support nighttime comfort by:
- Gentle evening movement to stimulate circulation
- Avoiding prolonged immobility before bed
- Maintaining stable blood sugar (if diabetic)
- Keeping bedroom temperature comfortable
- Elevating legs slightly if swelling contributes
These strategies support comfort — but they do not replace structured nerve evaluation.
The Most Important Takeaway
Neuropathy often feels worse at night due to reduced distraction, altered circulation, and circadian pain sensitivity.
Nighttime worsening does not automatically mean catastrophic progression.
However, increasing nighttime disruption over time may reflect advancing nerve dysfunction.
Untreated neuropathy commonly progresses.
But measurable improvements in nerve function — including reduced nighttime symptoms — are achievable, particularly when addressed earlier.
Protecting sleep protects function.
Timing matters.
Frequently Asked Questions
Q: Why does neuropathy burn more at night?
A: Reduced distraction and circadian pain sensitivity make symptoms more noticeable during rest.
Q: Is nighttime worsening a bad sign?
A: Not automatically. However, increasing severity over time may indicate progression.
Q: Can neuropathy-related sleep problems improve?
A: Yes. Improvements in nerve function often reduce nighttime symptom intensity.
Q: Does nighttime pain mean neuropathy is advanced?
A: Not necessarily. Stage depends on overall sensory function and balance, not nighttime intensity alone.
Next Step
If nighttime burning, tingling, or tightness is disrupting sleep, earlier evaluation often allows for more efficient intervention before sleep loss contributes to further functional decline.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Improving nerve function often improves sleep — and preserving sleep protects independence.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
- Melzack R, Wall PD. Pain mechanisms. Science.
- Gilron I et al. Circadian variation in neuropathic pain. Pain Medicine.