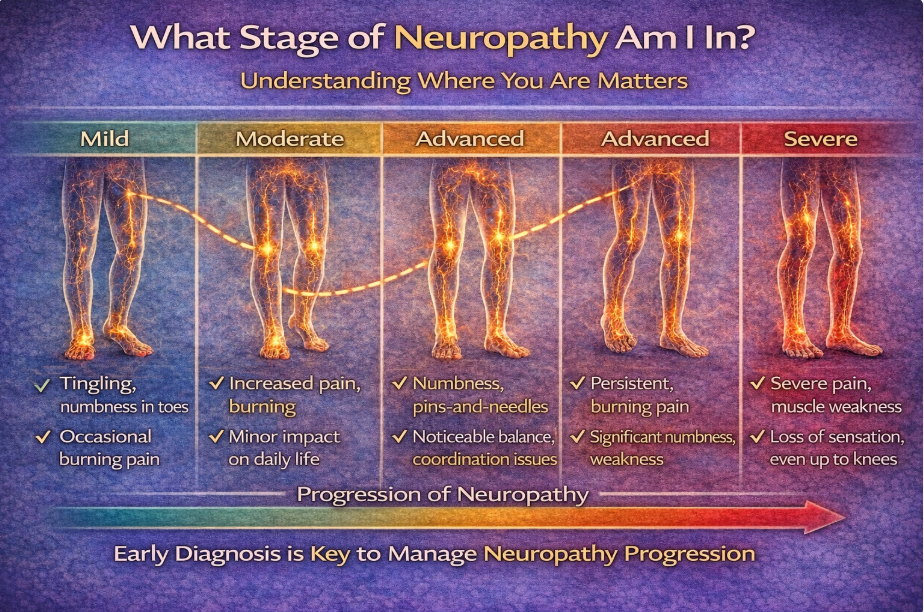
Many patients ask this question quietly:
“What stage am I in?”
They are not asking for a label.
They are asking:
Is this early?
Is this advanced?
Is this too late?
Can this still improve?
Neuropathy does not follow a universally accepted staging system like cancer.
But clinically, it does tend to follow recognizable patterns of progression.
Understanding where you are helps guide timing — and timing influences outcome.
Neuropathy Typically Progresses Gradually
Untreated peripheral neuropathy often progresses over time.
Symptoms commonly move in a length-dependent pattern:
- Toes
- Feet
- Calves
For more detail on progression timelines, see:
How Fast Does Neuropathy Progress?
While progression is common when unmanaged, the rate and functional impact vary.
Identifying stage helps determine how much function remains — and how much can still improve.
General Clinical Stages of Neuropathy
While not formally standardized, neuropathy often presents in recognizable phases.
Stage 1: Early Sensory Changes
Common features:
- Intermittent tingling
- Mild numbness
- Nighttime burning
- Subtle calf or arch tightness
- Normal walking but slight instability in the dark
At this stage:
- Protective sensation is partially intact
- Balance compensation is minimal
- Deconditioning has not yet developed
This stage is often overlooked because symptoms feel mild.
But this is also when measurable improvement tends to be most predictable.
Stage 2: Established Sensory Loss and Tightness
Common features:
- Persistent numbness
- More frequent burning
- Increased calf tightness
- Reduced vibration detection
- Noticeable balance shifts
- Avoidance of uneven surfaces
At this stage:
- Protective sensation is declining
- Compensation patterns are developing
- Walking endurance may decrease
Quality of life begins to change more noticeably.
This stage is still very responsive to structured intervention — but timing becomes more important.
Stage 3: Advanced Sensory Loss and Instability
Common features:
- Significant numbness
- Frequent imbalance
- Increased fall risk
- Reduced walking distance
- Deconditioning
- Possible autonomic involvement
For more on safety thresholds, see:
When Is Neuropathy Dangerous?
At this stage:
- Protective sensation may be significantly reduced
- Fall risk increases
- Compensatory tightness becomes chronic
- Deconditioning accelerates decline
Improvement is still possible.
But recovery tends to require more time and consistency.
Does Stage Determine Life Expectancy?
In most cases, neuropathy stage affects quality of life more than lifespan.
For clarification on mortality concerns, see:
What Is the Life Expectancy of a Person With Neuropathy?
Neuropathy rarely shortens life directly.
However, advanced-stage neuropathy increases risk of falls, inactivity, and functional decline.
Stage influences independence more than survival.
Can You Move Backward in Stage?
Peripheral neuropathy is typically progressive when untreated.
However, measurable improvements in nerve function are possible.
In clinical practice, improvement may include:
- Increased light-touch detection
- Improved vibration sense
- Reduced burning intensity
- Improved balance stability
- Increased walking endurance
- Reduced tightness
Earlier stages tend to show more predictable improvement than advanced stages.
This does not mean advanced cases cannot improve.
It means earlier intervention often produces more efficient results.
Nerve function is not fixed.
But timing matters.
Why Self-Diagnosing Stage Can Be Misleading
Symptoms do not always match nerve testing precisely.
Some patients with mild symptoms already have measurable deficits.
Others with more noticeable discomfort retain significant nerve function.
Structured evaluation provides more clarity than guesswork.
The Most Important Takeaway
Neuropathy does not come with a formal stage label.
But clinically, it progresses from subtle sensory change to more advanced instability if untreated.
Untreated neuropathy often advances over time.
However, measurable nerve function improvement is achievable — particularly when intervention begins earlier rather than later.
Stage influences how predictable improvement will be.
Timing shapes trajectory.
Frequently Asked Questions
Q: How do I know what stage my neuropathy is in?
A: Stage is determined by symptom pattern, sensory testing, and functional stability — not symptoms alone.
Q: Is early-stage neuropathy reversible?
A: Early-stage neuropathy is often more responsive to structured intervention and measurable improvement.
Q: Can advanced neuropathy improve?
A: Yes. Improvement is possible, but it typically requires more time and consistency.
Q: Does stage affect life expectancy?
A: Neuropathy stage primarily affects quality of life and fall risk, not lifespan directly.
Next Step
If you are unsure where your neuropathy stands — or if symptoms feel like they are gradually advancing — earlier evaluation often allows for more efficient intervention before instability and deconditioning become entrenched.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Preserving function earlier is typically easier than restoring it after long-standing decline.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
- England JD et al. Distal symmetric polyneuropathy. Neurology.
- Richardson JK. Peripheral neuropathy and fall risk. Mayo Clinic Proceedings.