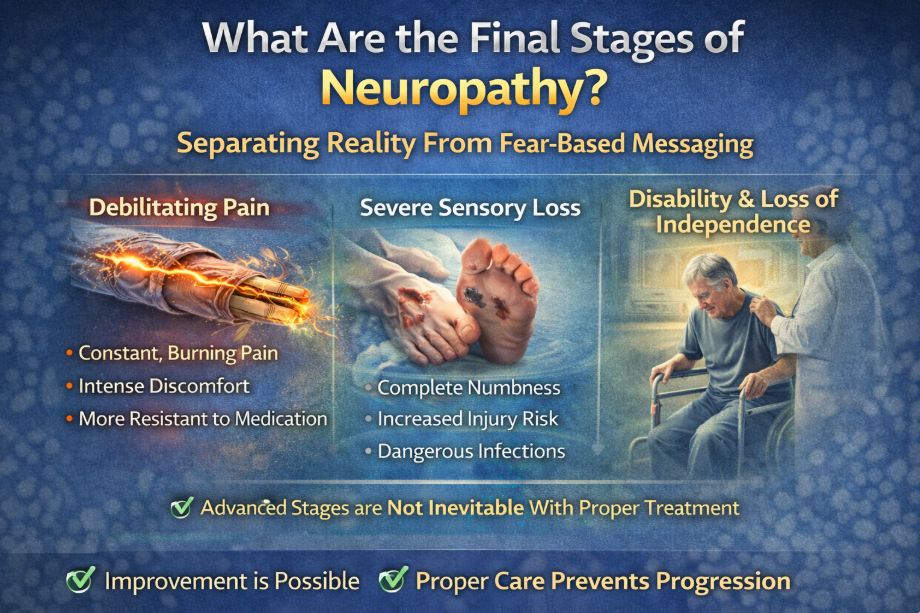
When people search for “final stages of neuropathy,” they are usually scared.
Many have seen advertisements claiming:
“If you do nothing, your feet will be amputated.”
That type of messaging is designed to create urgency.
But it often oversimplifies — and exaggerates — what actually happens.
Let’s clarify what advanced neuropathy really looks like.
First: Neuropathy Is Not a Terminal Disease
Peripheral neuropathy does not follow a predictable “terminal stage” like certain cancers.
It does not automatically lead to death.
For clarification on mortality concerns, see:
Can Neuropathy Cause Death?
When neuropathy progresses, it affects function — not life expectancy directly.
What “Advanced Neuropathy” Actually Means
Advanced neuropathy typically includes:
- Significant sensory loss
- Markedly reduced vibration detection
- Increased balance instability
- Frequent near-falls or falls
- Reduced walking endurance
- Persistent tightness
- Possible autonomic involvement
For staging details, see:
What Stage of Neuropathy Am I In?
Advanced neuropathy is characterized by functional limitation — not inevitability of amputation.
Where Amputation Risk Actually Comes From
Amputation risk is most strongly associated with:
- Diabetes
- Severe vascular disease
- Poor wound healing
- Undetected foot injuries
- Advanced infection
Loss of protective sensation increases risk of unnoticed injury.
However, neuropathy alone does not automatically lead to amputation.
Amputation typically occurs when multiple risk factors combine:
Neuropathy + poor circulation + ulcer + infection + delayed care.
That is a very different scenario than “neuropathy always leads to amputation.”
Why Fear-Based Advertising Is Misleading
Alarmist messaging often implies:
“If you don’t act immediately, you will lose your feet.”
This is not how neuropathy typically progresses.
Untreated neuropathy commonly advances gradually.
For progression details, see:
How Fast Does Neuropathy Progress?
The real concern in advanced neuropathy is:
- Loss of protective sensation
- Increased fall risk
- Reduced mobility
- Deconditioning
- Decreased independence
These are serious — but preventable — risks.
Fear does not improve outcomes.
Structured care does.
What Advanced Neuropathy Looks Like Clinically
In later stages, patients may experience:
- Severe numbness
- Difficulty feeling the floor
- Instability in low light
- Reduced reflex correction
- Calf tightness from compensation
- Reduced activity tolerance
Balance and strength can still improve — but advanced cases often require more structured rehabilitation.
Patients may need to:
- Rebuild strength
- Reinforce balance
- Gradually increase walking tolerance
- Reintroduce functional movement progressively
Improvement is achievable.
It simply requires consistency and guidance.
Can Advanced Neuropathy Improve?
Yes.
Peripheral nerves retain capacity for measurable improvement.
Even in advanced stages, patients may experience:
- Improved sensory detection
- Reduced burning intensity
- Increased balance stability
- Better walking endurance
However, earlier intervention tends to produce more predictable gains.
Advanced neuropathy does not equal hopelessness.
It means more structured rehabilitation is required.
What Truly Prevents Complications
Preventing severe complications involves:
- Regular foot monitoring
- Proper footwear
- Metabolic control
- Balance reinforcement
- Early wound care
- Structured nerve evaluation
Amputation risk is not automatic.
It is the result of unmanaged progression combined with other systemic risk factors.
The Most Important Takeaway
There is no universal “final stage” where neuropathy automatically leads to amputation.
Peripheral neuropathy primarily affects sensation and balance.
Untreated neuropathy commonly progresses.
But measurable improvements in nerve function and stability are achievable — even in advanced cases — particularly when addressed before severe deconditioning occurs.
Fear-based messaging oversimplifies the issue.
Proactive, structured care protects independence.
Timing matters.
Frequently Asked Questions
Is amputation inevitable with neuropathy?
No. Amputation risk is typically associated with diabetes, vascular disease, and untreated wounds — not neuropathy alone.
What happens in advanced neuropathy?
Severe sensory loss, instability, and reduced endurance may occur.
Can advanced neuropathy improve?
Yes. Improvement is possible but may require more structured rehabilitation.
Is neuropathy terminal?
No. Peripheral neuropathy rarely shortens lifespan directly.
Next Step
If you are concerned about progression — or have seen alarming claims about “final stages” — earlier structured evaluation often allows for more efficient intervention before instability and deconditioning advance.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Neuropathy does not automatically lead to amputation.
But proactive care protects independence.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.