One of the first questions patients ask is:
“How fast is this going to get worse?”
That question is rarely just about symptoms.
It’s about independence.
Mobility.
Balance.
Sleep.
Long-term function.
The honest answer is this:
Untreated peripheral neuropathy typically progresses over time.
But progression is not uniform — and it is not untouchable.
The more important question is not whether it progresses.
It’s whether the trajectory can be altered.
Neuropathy Is Often Progressive When Ignored
Peripheral neuropathy reflects ongoing stress to peripheral nerves.
In clinical practice, when contributing factors are not addressed, neuropathy tends to:
- Gradually worsen
- Spread in a length-dependent pattern
- Increase tightness and sensory loss
- Reduce balance stability
- Decrease walking endurance
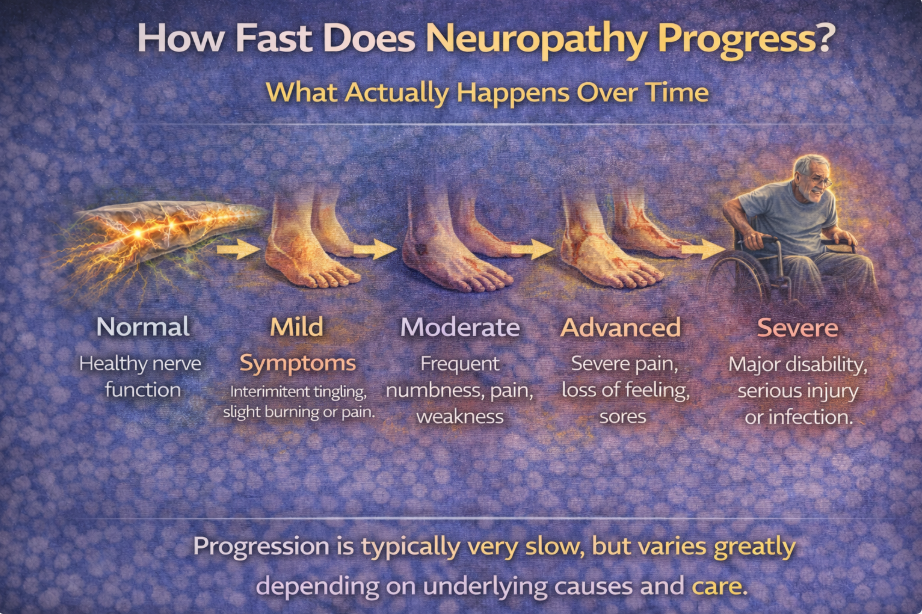
Most commonly, symptoms begin in the toes and move upward toward the feet and calves.¹
This occurs because longer nerves are more metabolically vulnerable.
Progression usually unfolds over months or years — not days.
The gradual nature often gives a false sense of safety.
Slow Progression Still Impacts Quality of Life
Even gradual change can significantly affect daily function.
Over time, untreated neuropathy can lead to:
- Reduced protective sensation
- Increased fall risk
- Chronic calf and arch tightness
- Deconditioning due to activity avoidance
- Sleep disruption
Neuropathy rarely shortens lifespan directly.
However, it can meaningfully reduce quality of life if allowed to progress unchecked.
For a broader discussion of long-term outlook and survival concerns, see:
What Is the Life Expectancy of a Person With Neuropathy?
That distinction matters.
Progression Is Influenced by the Underlying Cause
The speed of change depends on factors such as:
- Blood sugar control
- Vascular health
- Nutritional status
- Autoimmune activity
- Medication effects
- Overall metabolic health
If systemic stress continues, nerve dysfunction often advances.²
When patients ask whether neuropathy is life-threatening, that concern is usually tied to underlying disease — not nerve damage itself.
For clarification on that, see:
Is Neuropathy a Terminal Condition?
Addressing contributing factors early can meaningfully influence trajectory.
Peripheral Nerves Retain Capacity for Improvement
Peripheral nerve function is not fixed.
In clinical practice, measurable improvements in nerve function are possible — particularly when intervention begins earlier rather than later.
Improvement may include:
- Increased light-touch detection
- Improved vibration sense
- Reduced burning intensity
- Improved balance stability
- Increased walking endurance
- Reduced tightness
This does not mean neuropathy disappears overnight.
But it does mean the slope of decline can be altered.
Left alone, the curve trends downward.
Addressed early and systematically, the curve often flattens — and in many cases improves.
Treatment approach matters.
For more on how structured care influences outcomes, see:
How Do You Treat Neuropathy in the Feet?
Why Earlier Intervention Matters
After more than 20 years focused exclusively on neuropathy care, one pattern is consistent:
Earlier-stage neuropathy responds more predictably than advanced-stage neuropathy.
When sensation is mildly reduced:
- Compensatory patterns are less entrenched
- Deconditioning is less advanced
- Tightness is less chronic
- Balance deficits are less severe
Waiting until instability becomes pronounced or sleep is significantly disrupted makes recovery slower and more complex.
Progression does not have to be dramatic to be meaningful.
A small decline each year accumulates.
Earlier care changes that trajectory.
What About Sudden Worsening?
Patients sometimes experience symptom flares.
Common triggers include:
- Illness
- Blood sugar fluctuations
- Stress
- Sleep disruption
- Medication changes
Temporary flares do not necessarily represent permanent decline.
However, rapid weakness, sudden loss of coordination, or dramatic neurological changes are not typical of chronic neuropathy.
If you are concerned that symptoms are changing rapidly or unpredictably, see:
When Is Neuropathy Dangerous?
The Most Important Takeaway
Untreated peripheral neuropathy typically progresses.
But progression is not destiny.
Peripheral nerves retain the capacity for functional improvement — particularly when addressed earlier in the course of decline.
Neuropathy rarely shortens life directly.
However, it can significantly affect quality of life if ignored.
Earlier structured evaluation and intervention tend to produce more predictable and meaningful functional gains than waiting until symptoms are advanced.
Clarity supports better timing.
Frequently Asked Questions
Q: Does neuropathy always get worse?
A: When untreated, neuropathy commonly progresses over time. However, measurable nerve function improvement is possible with structured intervention.
Q: Can neuropathy improve?
A: Yes. Improvements in sensation, balance, and functional stability are achievable, particularly in earlier stages.
Q: How quickly does neuropathy spread?
A: Most chronic neuropathy progresses gradually over months or years.
Q: Is sudden worsening normal?
A: Temporary flares can occur. Rapid weakness or dramatic neurological changes require evaluation.
Next Step
If you have noticed gradual changes in sensation, balance, or tightness — even if they feel subtle — earlier evaluation often allows for more efficient intervention before deficits become advanced.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Addressing neuropathy earlier tends to produce more predictable functional improvement than waiting until instability is entrenched.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.