If you have peripheral neuropathy, you’ve probably searched for solutions.
TENS units.
Vitamin B12.
Alpha-lipoic acid.
Magnesium.
Topical creams.
Patients are often willing to try almost anything to reduce burning, numbness, tightness, or instability.
The important question is not whether these options exist.
It is whether they meaningfully change nerve function — or simply modify symptoms.
Understanding the difference matters.
What a TENS Unit Actually Does
TENS stands for Transcutaneous Electrical Nerve Stimulation.
These devices deliver low-level electrical impulses through the skin to stimulate sensory nerves.
The goal is typically pain modulation.
TENS works primarily through a mechanism known as the “gate control theory” of pain.¹ Electrical stimulation may temporarily interfere with pain signal transmission to the brain.
For some patients, this reduces discomfort.
But TENS does not regenerate nerve fibers.
It does not correct metabolic contributors.
It does not reverse structural damage.
It is a symptom-modulation tool.
That distinction is important.
When TENS May Be Helpful
TENS may provide temporary relief for:
- Burning sensations
- Sharp neuropathic pain
- Localized discomfort
Some studies show modest short-term improvement in neuropathic pain scores.²
However, results vary widely.
Relief often lasts only while the device is being used.
Patients should view TENS as a tool for symptom management — not a corrective therapy.
What About Interferential Therapy?
Interferential therapy (IFT) uses a different electrical pattern designed to penetrate deeper tissue.
Unlike basic TENS, interferential currents may reach deeper structures and may feel more comfortable at higher intensities.
Some patients report better tolerance with IFT compared to traditional TENS.
But again — electrical stimulation does not inherently repair nerve fibers.
It may influence perception, circulation, and tissue response.
The difference between symptom modulation and structural change should remain clear.
Supplements and Neuropathy: What Does the Evidence Say?
Supplements are widely marketed for neuropathy.
Some have supportive evidence. Others are overhyped.
Let’s separate them.
Vitamin B12
Vitamin B12 deficiency can cause neuropathy.³
If deficiency is present, correction is essential.
However, taking B12 in the absence of deficiency does not reliably improve neuropathy symptoms.
Testing matters.
Alpha-Lipoic Acid (ALA)
Alpha-lipoic acid has been studied in diabetic neuropathy.
Some clinical trials suggest modest symptom reduction at certain doses.⁴
However:
- Effects are variable
- Benefits may diminish when stopped
- Structural nerve regeneration is not clearly established
It may help some patients symptomatically.
It is not a universal solution.
Magnesium
Magnesium supports nerve excitability and muscle function.
However, evidence supporting magnesium as a primary neuropathy treatment is limited.
It may support general neuromuscular health but is not a targeted neuropathy therapy.
Other Common Supplements
Products containing:
- Acetyl-L-carnitine
- B-complex blends
- Herbal combinations
have mixed or limited evidence.
Some small studies suggest benefit.⁵ Many lack strong replication.
Patients should approach supplement claims cautiously.
The Difference Between Supporting Nerves and Repairing Nerves
This is the critical distinction.
Some interventions may:
- Reduce symptom intensity
- Improve circulation temporarily
- Modulate nerve excitability
Very few have strong evidence for true structural nerve regeneration in humans.
Improvement in sensation or balance typically requires structured, consistent intervention and monitoring.
Quick fixes are rare.
Why Patients Feel Confused
The supplement and device market is large.
Marketing often implies reversal.
Scientific literature is more nuanced.
Over more than 20 years focused exclusively on neuropathy care, one consistent observation stands out:
Patients benefit most when symptom tools are integrated into a structured plan rather than used randomly.
The Most Important Takeaway
TENS and certain supplements may reduce symptoms for some patients.
They do not replace thoughtful evaluation.
They do not substitute for structured monitoring.
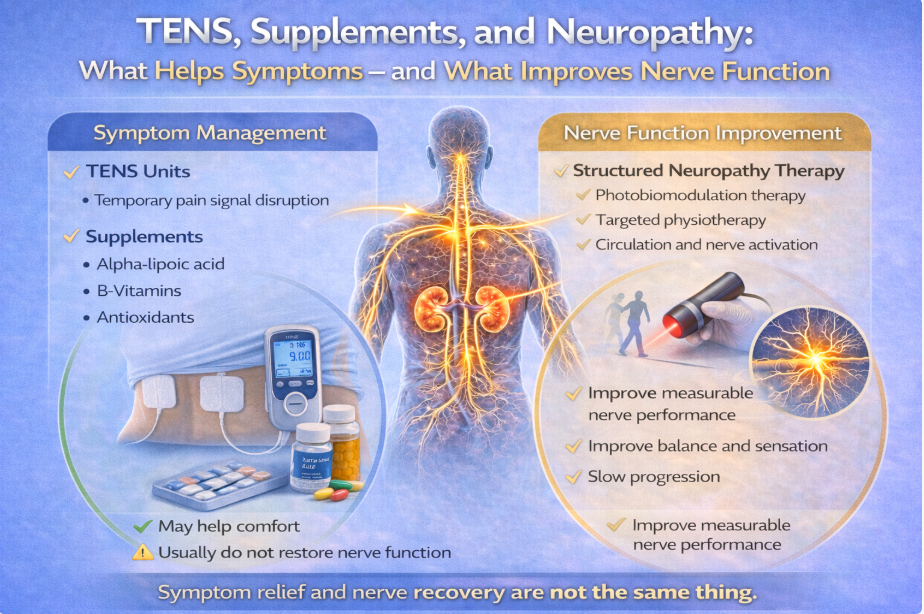
Symptom relief and nerve recovery are not the same thing.
Clarity allows better decisions.
Frequently Asked Questions
Q: Do TENS units cure neuropathy?
A: No. TENS units may temporarily reduce pain but do not repair damaged nerves.
Q: Is alpha-lipoic acid proven to reverse neuropathy?
A: Some studies show modest symptom improvement, particularly in diabetic neuropathy, but consistent structural reversal has not been established.
Q: Should I take B12 for neuropathy?
A: B12 should be taken if deficiency is present. Testing is recommended before supplementation.
Q: Are supplements enough to treat neuropathy?
A: Supplements alone rarely provide comprehensive management. Structured evaluation and monitoring remain important.
Next Step
If you are using TENS, supplements, or other symptom-based tools but still feel uncertain about progression, a structured neuropathy evaluation can help clarify what is helping, what is not, and what your symptoms may represent.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Early clarity can influence long-term trajectory.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
- Melzack R, Wall PD. Pain mechanisms: a new theory. Science.
- Johnson MI et al. Transcutaneous electrical nerve stimulation for neuropathic pain. Cochrane Review.
- O’Leary F, Samman S. Vitamin B12 deficiency and neurological disease. Nutrients.
- Ziegler D et al. Alpha-lipoic acid in diabetic neuropathy. Diabetes Care.
- Bril V et al. Evidence-based guideline: Treatment of painful diabetic neuropathy. Neurology.