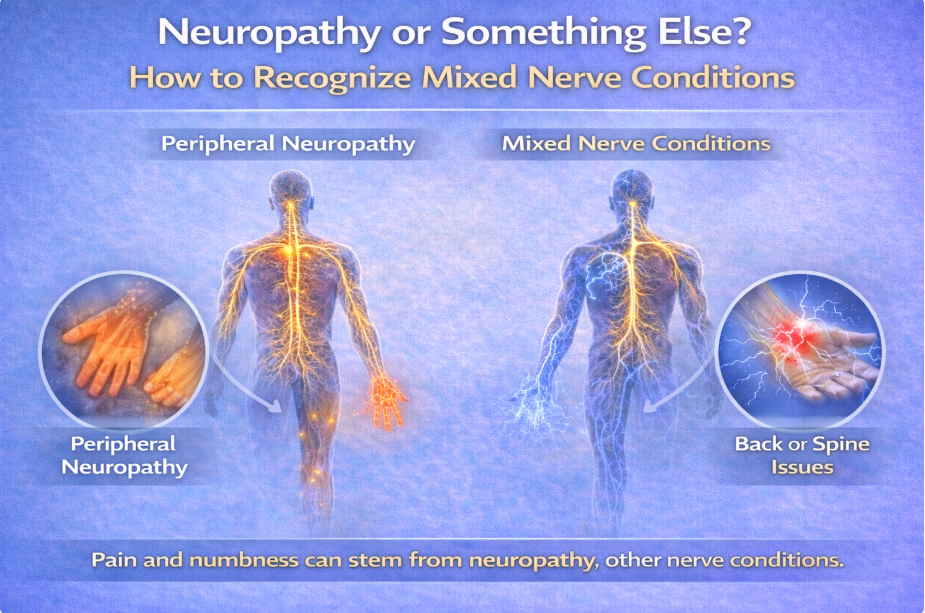
Burning. Numbness. Tingling. Tightness. Instability.
When symptoms appear in the feet or legs, many patients are quickly told they have “peripheral neuropathy.”
Sometimes that diagnosis is accurate.
Sometimes it is incomplete.
And sometimes — it is both.
After more than 20 years focused exclusively on neuropathy evaluation and treatment, one pattern has become clear:
Mixed conditions are far more common than isolated ones.
Understanding that distinction changes how symptoms are interpreted and how care should be structured.
What Classic Peripheral Neuropathy Looks Like
Peripheral neuropathy most often follows a length-dependent pattern.¹
This means:
- Symptoms begin in the toes
- Progress upward gradually
- Affect both sides symmetrically
Long nerve fibers are more metabolically vulnerable, which explains why the feet are typically affected first.
When symptoms do not follow this pattern, additional contributors should be considered.
Clues That Suggest More Than Neuropathy Alone
Certain features raise suspicion that overlapping conditions may be present.
Marked asymmetry
If one leg is significantly worse than the other, structural or vascular factors may be contributing.
Radiating pain from the lower back
Sharp or shooting pain traveling down the leg may suggest nerve root irritation, also called radiculopathy.²
Symptoms that change with position
If sitting, standing, bending, or walking alters symptoms dramatically, spinal or mechanical drivers may be involved.
Sudden worsening
Classic neuropathy progresses gradually. Rapid changes may indicate a new overlay rather than simple progression.
These distinctions matter.
Common Overlapping Contributors
In clinical practice, it is common to see neuropathy coexist with:
- Lumbar spinal stenosis
- Disc-related nerve root irritation
- Peripheral nerve entrapments
- Vascular insufficiency
- Medication-related nerve effects
- Autonomic dysfunction
For example, a patient may have small fiber neuropathy causing baseline burning and numbness, while also having lumbar nerve root compression contributing to weakness or asymmetry.
If only one issue is addressed, improvement remains limited.
Why Mixed Conditions Are Frequently Missed
Healthcare is often segmented.
The spine is evaluated separately from neuropathy.
Circulation is evaluated separately from neurological function.
Medication effects are reviewed independently.
Without pattern integration, overlapping drivers are easily overlooked.
This can lead to:
- Partial treatment
- Persistent symptoms
- Frustration despite “correct” diagnosis
Care improves when evaluation integrates rather than isolates.
The Role of Tightness in Mixed Conditions
Tightness is often misclassified as purely muscular.
But persistent calf or arch tightness may reflect:
- Autonomic dysregulation
- Altered vascular tone
- Sensory nerve hypersensitivity
- Protective compensation due to instability
When neuropathy and structural contributors coexist, tightness may become amplified.
Addressing only the muscular component rarely provides durable relief.
Structured evaluation helps determine whether tightness is mechanical, neurological, or both.
Why Accurate Differentiation Matters
When contributors are properly identified:
- Treatment becomes more targeted
- Expectations become realistic
- Progress can be measured appropriately
Not every foot symptom is “just neuropathy.”
And not every neuropathy case is isolated.
Clarity prevents chasing the wrong problem.
The Most Important Takeaway
Neuropathy is real.
So are structural, vascular, and autonomic overlays.
When symptoms do not fit neatly into one category, simplification is not helpful.
Thoughtful differentiation is.
Frequently Asked Questions
Q: Can neuropathy and a back problem happen together?
A: Yes. Lumbar nerve root irritation and peripheral neuropathy frequently coexist.
Q: Why are my symptoms worse on one side?
A: Significant asymmetry often suggests structural, vascular, or entrapment-related contributors in addition to neuropathy.
Q: How do doctors tell the difference between neuropathy and radiculopathy?
A: Pattern distribution, symmetry, positional influence, reflex testing, and neurological examination help differentiate the two.²
Q: Can neuropathy be misdiagnosed?
A: Symptoms can overlap with spine, vascular, or medication-related conditions. Careful evaluation improves diagnostic clarity.
Next Step
If your symptoms do not fit a clear pattern — or if you have received multiple explanations without clarity — a structured neuropathy evaluation can help determine whether overlapping conditions are present and which contributors are dominant.
To learn more or request a consultation at Realief Neuropathy Centers of Minnesota, call 952-456-6160 or submit a request through our website.
Early clarity can influence long-term trajectory.
About the Author
Dr. Timothy Kelm is the founder of Realief Neuropathy Centers of Minnesota and has spent over 20 years focused exclusively on the evaluation and treatment of peripheral neuropathy. He has worked with thousands of neuropathy patients and delivered tens of thousands of neuropathy-focused treatments.
He is associated with published clinical research conducted in collaboration with the University of Minnesota and holds a nationally issued patent related to neuropathy treatment methodology. He has delivered public educational presentations and trained physicians nationally on structured neuropathy care.
Over 20 years ago, his interest in neuropathy began after repeatedly seeing patients who were told there were no good options. He believed then — and continues to believe today — that neuropathy should not define your life.
References
- England JD et al. Distal symmetric polyneuropathy. Neurology.
- Tarulli AW, Raynor EM. Radiculopathy and peripheral neuropathy differentiation. Neurol Clin.